13/10/2024
For professional drivers in the UK, particularly those in the demanding world of taxi services, maintaining optimal health is not just a personal choice but a professional imperative. When managing health conditions like diabetes, the medication you take can have significant implications for your ability to drive safely and legally. One such medication, Gliclazide, is commonly prescribed for Type 2 diabetes, and understanding its effects and the necessary precautions is paramount for every taxi driver. This comprehensive guide aims to equip you with the knowledge and practical advice needed to navigate your professional life safely and confidently while on Gliclazide, ensuring you meet both your health needs and your responsibilities on the road.

Driving a taxi requires constant vigilance, quick reflexes, and sustained concentration. These attributes can be compromised if your blood sugar levels are not well-controlled, especially if they drop too low, a condition known as hypoglycaemia. Gliclazide, by its very mechanism, carries a risk of causing hypoglycaemia, which is why strict adherence to specific protocols is not just recommended but essential. This article will delve into the specifics of driving with Gliclazide, compare it with other diabetes treatments, and crucially, provide actionable advice straight from healthcare professionals to help you stay compliant, safe, and protected in your vital role.
- Understanding Gliclazide and its Role in Diabetes Management
- Driving a Taxi on Gliclazide: Essential Protocols for Safety and Compliance
- The Legal and Societal Landscape: Protecting Your Livelihood
- Managing Your Diabetes: Beyond the Wheel
- Frequently Asked Questions for Taxi Drivers on Gliclazide
- Can I stop taking Gliclazide if my blood sugar levels are looking good?
- What should I do if I start to feel hypoglycaemic while driving?
- Do I need to inform the DVLA if I'm taking Gliclazide for diabetes?
- How often should I see my doctor or diabetic nurse about my Gliclazide prescription and driving?
- What are the common symptoms of hypoglycaemia I should be aware of?
- What kind of written record should I keep, and for how long?
- Conclusion: Drive Safely, Drive Responsibly
Understanding Gliclazide and its Role in Diabetes Management
Gliclazide is a widely prescribed oral medication for individuals with Type 2 diabetes. It belongs to a class of drugs known as sulfonylureas. Its primary function is to stimulate the beta cells in your pancreas to produce and release more insulin. Insulin is the hormone responsible for lowering blood sugar levels by helping glucose enter your body's cells for energy or storage. By increasing insulin production, Gliclazide effectively helps to bring elevated blood sugar levels down to a healthier range.
While Gliclazide can be a very effective treatment, its mechanism of action means it can sometimes lower blood sugar levels too much, leading to hypoglycaemia. This is a critical consideration for anyone, but especially for professional drivers, as the symptoms of low blood sugar can impair judgment, coordination, and reaction times, posing a serious risk to road safety. It's often prescribed when lifestyle changes alone are insufficient, or when other first-line medications like metformin are not suitable or no longer provide adequate blood sugar control on their own. Gliclazide can be used as a standalone treatment or in combination with other anti-diabetic medications to achieve optimal glucose management.
Gliclazide vs. Other Diabetes Medications: A Brief Comparison
Diabetes management is highly individualised, and there are various classes of medications available, each working differently to control blood sugar. Understanding how Gliclazide fits into this landscape can provide context for its specific driving implications. Here's a brief comparison with some other common diabetes medicines:
| Medicine Class | Example | How it Works | Driving Implications (General) |
|---|---|---|---|
| Biguanides | Metformin | Decreases glucose production by the liver and improves insulin sensitivity. | Low risk of hypoglycaemia when used alone. Generally very safe for driving. |
| Thiazolidinediones | Pioglitazone | Increases insulin sensitivity in muscle and fat tissue. | Low risk of hypoglycaemia when used alone. Generally safe for driving. |
| DPP-4 Inhibitors | Saxagliptin | Increase levels of 'incretin' hormones, which stimulate insulin release and reduce glucose production after meals. | Low risk of hypoglyphaemia when used alone. Generally safe for driving. |
| SGLT2 Inhibitors | Dapagliflozin | Cause the kidneys to remove more glucose from the body through urine. | Low risk of hypoglycaemia when used alone. Generally safe for driving. |
| GLP-1 Agonists | Exenatide | Mimic natural hormones that stimulate insulin release, slow digestion, and reduce appetite. | Low risk of hypoglycaemia when used alone. Generally safe for driving. |
| Sulfonylureas | Gliclazide, Glibenclamide, Glimepiride, Glipizide, Tolbutamide | Stimulate the pancreas to produce more insulin. | Significant risk of hypoglycaemia. Strict monitoring and precautions are essential for driving. |
| Insulin | Various types | Directly replaces or supplements the body's natural insulin. | Significant risk of hypoglycaemia. Requires strict monitoring and adherence to DVLA guidelines. |
As you can see, Gliclazide, along with other sulfonylureas and insulin, stands out due to its higher propensity to cause hypoglycaemia. This is precisely why specific precautions are vital for taxi drivers taking this medication. While other sulfonylureas like glibenclamide, glimepiride, glipizide, and tolbutamide work in a similar fashion, Gliclazide is often favoured due to a generally lower risk of severe hypoglycaemia compared to some older sulfonylureas, but the risk is still present and requires vigilance.
Driving a Taxi on Gliclazide: Essential Protocols for Safety and Compliance
The core question for any taxi driver on Gliclazide is: "Can I drive?" The answer is a resounding yes, provided you adhere strictly to established safety protocols. These aren't just suggestions; they are crucial measures to protect your own health, the safety of your passengers and other road users, and your professional livelihood. Furthermore, they are often implicitly, if not explicitly, tied to your legal responsibilities as a driver with a medical condition.
It's vital to remember that as a professional driver in the UK, you have a duty to inform the DVLA (Driver and Vehicle Licensing Agency) if you have diabetes managed with medication that carries a risk of hypoglycaemia, such as Gliclazide. While the initial diagnosis might have been communicated years ago, understanding the ongoing requirements is paramount. My nurse, a highly experienced professional in diabetic care, has highlighted the following critical points, which are reinforced by real-world experiences where drivers' adherence to these rules proved invaluable in unforeseen circumstances:
1. Pre-Drive Blood Glucose Check: Your First Line of Defence
Before you even put the key in the ignition or start your meter, you must check your blood glucose (BG) level. This is non-negotiable for a professional driver on Gliclazide. Your nurse advises:
- If your blood glucose is under 4.0 mmol/L: You must not drive. Instead, consume a fast-acting carbohydrate (like glucose tablets, a sugary drink, or a small snack). Wait for 30-45 minutes, then retest your blood glucose. Only if your reading is 4.0 mmol/L or above, and you feel well, can you consider driving. This waiting period is crucial to allow your body to absorb the sugar and for your levels to stabilise.
- If your blood glucose is 4.0 mmol/L or above: You are generally fine to drive. However, always consider how you feel. If you're feeling unwell, shaky, or experiencing any symptoms of hypoglycaemia despite a reading above 4.0 mmol/L, it's safer to delay driving until you feel completely well.
This initial check sets the tone for your entire shift. It ensures you begin your journey with stable blood sugar levels, significantly reducing the immediate risk of a hypoglycaemic episode behind the wheel.
2. Regular In-Drive Blood Glucose Monitoring: Ongoing Vigilance
Driving for extended periods can be tiring and stressful, both of which can impact blood glucose levels. Therefore, continuous monitoring throughout your shift is essential. The guidance is clear:
- Test every 2 hours while driving: Pull over safely to a suitable location (e.g., a service station, a designated rest area) and perform a blood glucose check. Do not attempt to test while driving, as this is a dangerous distraction.
- Follow the same protocol as your pre-drive check: If your reading is under 4.0 mmol/L, stop driving immediately, treat the low, wait 30-45 minutes, retest, and only resume driving if your BG is 4.0 mmol/L or above and you feel well.
- Adjust for long journeys: If you anticipate a very long shift or journey, plan your stops and checks accordingly. It's better to over-check than to risk a hypoglycaemic event.
This continuous monitoring ensures that any downward trend in your blood sugar can be caught and addressed before it becomes a dangerous situation. It demonstrates a proactive approach to managing your condition.
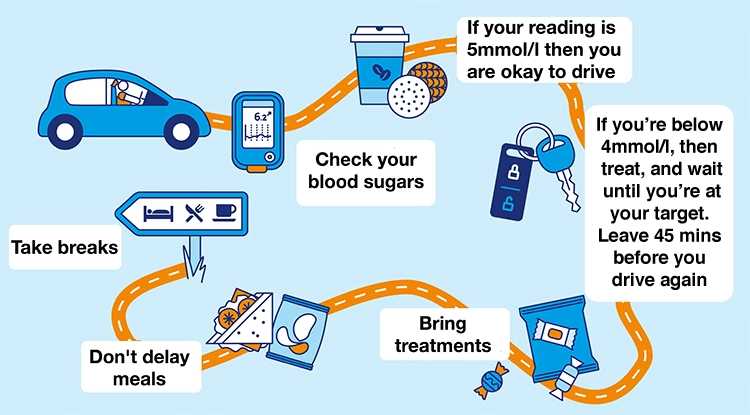
3. Always Carry Emergency Supplies: Food and Drink
Hypoglycaemia can strike unexpectedly, even with diligent monitoring. Having immediate access to treatment is vital. You must:
- Always carry fast-acting carbohydrates: Glucose tablets are ideal as they are precise and quick-acting. Sugary drinks (not diet drinks) like fruit juice or regular cola are also effective. Keep these within easy reach in your taxi.
- Carry longer-acting carbohydrates: Once you've treated a low with fast-acting carbohydrates, you'll need something more substantial to prevent your blood sugar from dropping again. Biscuits, a sandwich, or a piece of fruit can serve this purpose.
- Ensure you have water: Staying hydrated is generally good for health and can help you feel better.
Think of these supplies as your emergency kit. Just as you wouldn't drive without fuel, you shouldn't drive without your hypoglycaemia treatment.
4. Maintain a Meticulous Written Record of Readings
This point cannot be stressed enough, especially for professional drivers. In our increasingly litigious society, detailed documentation can be your strongest defence. You must:
- Keep a logbook: Record the date, time, and your blood glucose reading for every check you perform (before driving and every two hours during driving).
- Note any hypoglycaemic episodes: If you experience a low, record the reading, what you ate to treat it, the time you retested, and the subsequent reading.
- Carry this record with you: It should be readily available in your taxi.
The nurse highlighted situations where this meticulous record-keeping saved diabetic drivers from unwarranted blame after accidents. If you're involved in an incident, and there's a claim that your diabetes contributed, your records provide concrete evidence of your adherence to safety protocols. They can prove to police or insurance companies that you were driving responsibly and within the guidelines, even if your condition was brought into question.
5. Always Have Your Meter with You
This ties into the previous point about record-keeping and accountability. Your blood glucose meter is an indispensable tool, and it must be with you at all times when you're driving your taxi. The nurse explicitly mentioned cases where:
- Police may ask you to check your levels: In the event of a traffic stop or, more critically, an accident, police officers are increasingly aware of the implications of medical conditions on driving. They may request that you demonstrate your blood glucose level on the spot. Having your meter and being able to comply immediately shows responsibility and transparency.
- It reinforces your commitment to safety: Being able to produce your meter and logbook on demand sends a clear message that you are a responsible driver who takes your health and public safety seriously.
Your meter is not just for your personal use; it's a vital piece of equipment that serves as objective proof of your adherence to safe driving practices.
The Legal and Societal Landscape: Protecting Your Livelihood
The nurse's anecdote about individuals "looking for an excuse to get out of paying in an accident" is a sobering reminder of the legal vulnerabilities professional drivers face. In the aftermath of a road traffic incident, especially one involving personal injury, every detail can be scrutinised. If you have a known medical condition like diabetes, it's almost guaranteed that your health status and its management will be brought into question. This is not about guilt but about liability.
The cases cited by the nurse, where diabetic drivers were initially blamed until police investigation proved otherwise, underscore the importance of being beyond reproach. By diligently following the five protocols outlined above, you are not just managing your diabetes; you are building an irrefutable defence. Your written records, consistent blood glucose levels, and preparedness demonstrate that you took all reasonable steps to ensure you were fit to drive. This proactive approach can save you immense stress, legal fees, and potential professional repercussions.
Remember, the DVLA sets out clear guidelines for drivers with diabetes treated with medication that can cause hypoglycaemia. Failing to comply with these guidelines could not only lead to prosecution but also invalidate your insurance, putting your vehicle, your livelihood, and your financial security at severe risk. Your commitment to these safety measures is a testament to your professionalism and responsibility.
Managing Your Diabetes: Beyond the Wheel
While this article focuses on driving, it's crucial to remember that effective diabetes management is a 24/7 commitment. Your overall health and consistent blood sugar control will directly impact your ability to drive safely. This includes:
- Consistent medication adherence: Take your Gliclazide as prescribed by your doctor. Do not skip doses or alter them without medical advice.
- Healthy diet: Regular, balanced meals help to prevent large fluctuations in blood sugar. Avoid skipping meals, especially before or during long shifts.
- Regular physical activity: Even moderate exercise helps improve insulin sensitivity.
- Adequate sleep: Fatigue can affect your blood sugar levels and your ability to respond to hypoglycaemia.
- Stress management: The demands of taxi driving can be stressful. Find healthy ways to manage stress, as it can impact blood glucose.
These lifestyle factors contribute significantly to stable blood sugar, which in turn reduces the risk of hypoglycaemia and enhances your safety on the road.

Frequently Asked Questions for Taxi Drivers on Gliclazide
Can I stop taking Gliclazide if my blood sugar levels are looking good?
Absolutely not. You should never stop taking Gliclazide, or any diabetes medication, without first discussing it thoroughly with your GP or diabetic nurse. Stopping medication abruptly can lead to dangerously high blood sugar levels, which can cause severe health complications. Any adjustments to your treatment plan must be made under professional medical supervision.
What should I do if I start to feel hypoglycaemic while driving?
Your immediate priority is safety. As soon as you recognise the symptoms (shakiness, sweating, confusion, dizziness, blurred vision), pull over to the safest possible spot as quickly as you can. Turn off the engine. Do not attempt to continue driving. Treat the low blood sugar with fast-acting carbohydrates, wait until you feel fully recovered and your blood glucose is above 4.0 mmol/L, and then continue your journey.
Do I need to inform the DVLA if I'm taking Gliclazide for diabetes?
Yes, if you have diabetes and are treated with medication that carries a risk of hypoglycaemia (like Gliclazide), you are legally required to inform the DVLA. This applies to both private and professional driving licenses. Failure to do so can result in fines and the invalidation of your insurance.
How often should I see my doctor or diabetic nurse about my Gliclazide prescription and driving?
Regular check-ups are essential. Your GP or diabetic nurse will advise on the frequency, but typically, you should have reviews at least once a year, and often more frequently, especially if your blood sugar control is fluctuating, or if you are experiencing frequent hypoglycaemic episodes. These appointments are crucial opportunities to discuss your driving safety and any concerns you might have.
What are the common symptoms of hypoglycaemia I should be aware of?
Being able to recognise the early signs of hypoglycaemia is critical. Symptoms can include: feeling shaky or trembling, sweating, anxiety or irritability, hunger, light-headedness or dizziness, blurred vision, difficulty concentrating, confusion, slurred speech, and extreme tiredness. If you experience any of these, act immediately by pulling over and treating the low blood sugar.
What kind of written record should I keep, and for how long?
A small notebook or a dedicated logbook is ideal. Record the date, time, and your blood glucose reading for every test, especially before and during driving. Also, note any instances of hypoglycaemia, what you did to treat it, and the time and result of your retest. Keep these records for at least a year, or as advised by your healthcare professional, as they may be required by the DVLA or insurance companies in certain situations.
Conclusion: Drive Safely, Drive Responsibly
Being a taxi driver on Gliclazide is entirely possible and common, but it comes with significant responsibilities. The key to maintaining your safety, the safety of your passengers, and your professional standing lies in diligent self-management and strict adherence to the protocols advised by your healthcare team. By consistently checking your blood glucose, carrying emergency supplies, and meticulously recording your readings, you are not only managing your diabetes effectively but also building a robust defence against potential liabilities. Your proactive approach to health and safety is a mark of a true professional. Always remember to maintain open communication with your GP and diabetic nurse; they are your primary resource for ensuring your health supports your vital role on the roads of the UK.
If you want to read more articles similar to Gliclazide & Driving: UK Taxi Safety Guide, you can visit the Taxis category.

